The week of Columbus Day 2014 began with Beth and John Dorsa visiting Beth’s OB/GYN for a routine ultrasound. Beth was just over 23 weeks pregnant and everything appeared to be progressing normally. The ultrasound went well but the doctor wanted to check the baby’s weight since she had gestational diabetes. This is done to ensure that the baby doesn’t get too big. Beth scheduled an appointment to have it done later in the week at the hospital.
The week moved along as usual. Beth and John began telling their respective offices that they were expecting. Beth remained active throughout her pregnancy, even walking four miles on Thursday of that week.
Friday, October 17 began as a picture perfect day. John left for Manhattan, where he worked, while Beth worked from home in the morning. At at noon she went to Old Navy to purchase some maternity pants since she hadn’t begun to wear maternity clothes. Her ultrasound appointment was scheduled for 3 PM that day.
Beth was relaxed and heard the heartbeat during the ultrasound, however the technician excused herself to speak with a doctor. The Doctor entered the room and informed Beth that the ultrasound had revealed a deficiency in amniotic fluid and they would be taking her to Labor and Delivery immediately. She was told there could be at least three possible reasons: Beth’s water broke, the baby’s kidneys were not functioning properly, or the placenta was not functioning properly. John was notified and rushed to the hospital.
While in Labor and Delivery, it was determined that the placenta was not functioning and Beth should be admitted for monitoring. The expectation was to keep Beth in the Hospital for at least a few more weeks to prolong the pregnancy and give the baby the best odds for a positive outcome.
By 9 PM the couple decided that John should go home and grab some clothes for Beth since it was clear she would remain in the hospital for at least few weeks. They were informed that Beth’s stay would be tied to the Baby’s heartbeat; if it were strong, she would be released. If it dipped, they would consider taking additional measures.
John returned to the hospital about an hour later. At 10:15 the doctors rushed in because the baby’s heart rate had dropped and they indicated that the baby would have to be delivered immediately. John was placed in scrubs, however he was not allowed in the operating room. Beth was put under general anesthesia.
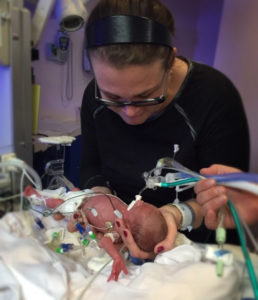
At 10:30 John received the initial news in the form of a Nurse handing him his daughter’s footprints and word from the doctor that Beth was stable and that they were working on their daughter. Scarlett Jane was born at 23 weeks and 6 days weighing 540 grams (1.19 pounds). She began breathing on her own but was quickly rushed to the NICU where she was placed on a ventilator.

For the next 117 days Beth and John called the North Shore NICU their home. They shared Halloween, Thanksgiving, Hanukkah, Christmas, and New Years with other families, nurses and doctors.
They cheered Scarlett Jane along and shared the triumph when she was finally able to come off of the ventilator, along with the frightening uncertainty of knowing she had a bilateral grade-three brain bleed.
With every positive step forward, another seemingly difficult obstacle laid ahead. Through countless heel pricks, numerous blood transfusions, a PDA ligation, three Retina of Prematurity laser treatments and re-intubations, Scarlett Jane handled everything that was thrown at her. A year after her birth, Scarlett Jane Dorsa weighed over 17 pounds.
